 Scientists at Johns Hopkins University (Baltimore, USA) are busy working on a new anti-obesity treatment that involves injecting microscopic beads into the stomach. The procedure has already been tested on a group of severely obese volunteers and the scientists who conducted the trial say the treatment is minimally invasive and safe.
Scientists at Johns Hopkins University (Baltimore, USA) are busy working on a new anti-obesity treatment that involves injecting microscopic beads into the stomach. The procedure has already been tested on a group of severely obese volunteers and the scientists who conducted the trial say the treatment is minimally invasive and safe.
The new technique, called bariatric arterial embolization, works by reducing grelin levels. Although it is often referred to as “the hunger hormone”, grelin is not the only hormone that effects the appetite. In actual fact the body produces two hunger hormones. The other one is leptin and it’s a figure-friendly hormone because it decreases the appetite. Grelin works in the opposite way. It’s an appetite increaser that is primarily released in the stomach and sends hunger signals to the brain.
[info]Bariatric Arterial Embolisation is similar in concept to Liraglutide, which will be marketed under the name Saxenda. Saxenda is made in Denmark by industry specialists Novo Nordisk, the drug will be sitiated inside an injectable pen similar to that used by diabetics
Click here to read more on Saxenda liraglutide[/info]
If bariatric arterial embolization is eventually approved as a weight loss treatment it could have the potential to improve a lot of lives. Obesity is a global problem and, apart from the health risks it poses to the inflicted individuals, it also places a costly burden on the World’s health care systems. In the UK it has been estimated that the treatment of obese patients cost the NHS £4.2 billion in 2007 and the Modelled projection for 2015 was £27 billion.
The anti-obesity measures that are commonly used at the moment are:
- Behavioural modifications
- Medication/supplements
- Diet and exercise
- Surgical procedures (gastric band etc.)
Speaking about the benefits of bariatric arterial embolisation, Director of Interventional Radiology Research at Johns Hopkins, Dr Clifford Weiss said: “We’re excited about the possibility of adding bariatric arterial embolization as another tool for health care providers to offer patients in the effort to curb this [obesity] epidemic.”
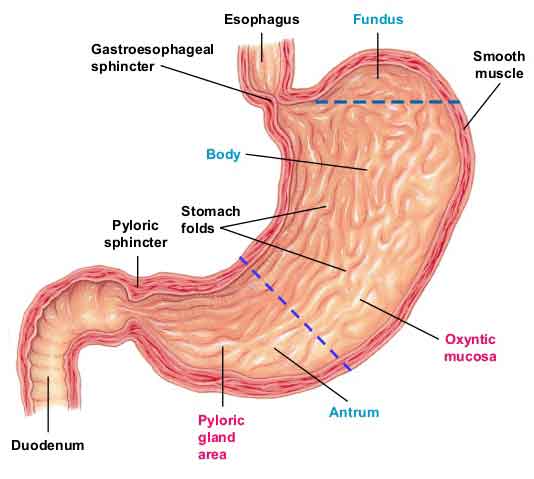
Most of the body’s supply of grelin is produced in a part of the stomach called the fundus, which is located in near the oesophagus; so the beads, which are introduced to the body via a small catheter, target this area.
For the purposes of an early clinical trial called Bariatric Embolization of Arteries for the Treatment of Obesity (BEAT), the researchers recruited one man and six women (aged 31 to 59). Anyone who has a (BMI) of 30 or more is classed as obese. The BMI of the seven volunteers ranged from 40 to 50, but although they were severely obese they were in good health.
Prior to receiving bariatric arterial embolization, the volunteers were educated about the various ways they could change their diet and improve their lifestyle.
The scientists believed the beads would decrease blood flow in the area, causing grelin production to be reduced, thereby suppressing the appetite.
The study had a duration of six months and the the scientists kept a careful note of the volunteers’ response to the treatment.
The areas of particular interest were:
- Grelin levels
- Weight loss
- Hunger and satiety
- Adverse reactions
The resulting data showed all seven of the volunteers experienced “dramatic huger reduction levels“.
 After two weeks of treatment the volunteers reported (via questionnaires) an average reduction in hunger of 81%. After one month the average hunger reduction was 59%, and by the time they had been receiving bariatric arterial embolization for three months the average hunger reduction was 26%. By this time the volunteers’ grelin levels had dropped by an average of 17.5%.
After two weeks of treatment the volunteers reported (via questionnaires) an average reduction in hunger of 81%. After one month the average hunger reduction was 59%, and by the time they had been receiving bariatric arterial embolization for three months the average hunger reduction was 26%. By this time the volunteers’ grelin levels had dropped by an average of 17.5%.
Sharing his opinion about the results of the study, Dr Weiss said they demonstrate bariatric arterial embolization is a safe procedure that appears to be effective for “helping patients lose a significant amount of weight in the short and intermediate term”.
“Compared to a surgical gastric bypass procedure,” Weiss continued, “bariatric arterial embolization is significantly less invasive and has a much shorter recovery time.”
Research is still in the early stages and further clinical trials will be needed, involving a larger number of people, but the early results are promising and studies are also being carried out at Mount Sinai Health System in New York.
Read about Compound 14 – a molecule that can speed up the metabolism

Be the first to comment